|
12/11/2023 0 Comments Adult tidal volume chart
In this case, the trend of the EtCO2 may be more useful that the absolute value and a blood gas may be required periodically to assess the difference between EtCO2 and PCO2 in the blood.ĮtCO2 can be useful in weaning mechanical ventilation and initiation of trials off the ventilator in patients with tracheostomies. Since many of the patients we care for on mechanical ventilators have diseases that affect either the pulmonary parenchyma or the pulmonary vasculature, they often have significantly increased alveolar dead space, which leads to a greater difference between PACO2 and EtCO2. We can generally expect EtCO2 to be an acceptable estimate of alveolar PCO2 (PACO2) in normal subjects however, the difference between the EtCO2 and PACO2 can be quite large in patients with diseased lungs. We commonly use EtCO2 to confirm proper endotracheal tube placement, assess the quality and effectiveness of cardiopulmonary resuscitation, and monitor for ventilation changes. End-tidal CO2 (EtCO2), which provides a measurement of CO2 concentration in exhaled gas, can help us monitor the adequacy of perfusion and ventilation. Significant hypercarbia may not cause desaturation on pulse oximetry until very late in a patient receiving supplemental oxygen or manifest as a change in mental status if the patient receives sedative medications. If we do not provide adequate ventilation to patients, they can develop hypercarbia, leading to respiratory acidosis and cardiovascular collapse. 4,5 Therefore, targeting an SpO2 of 94-98% in most patients requiring mechanical ventilation best balances the risks of both hypoxia and hyperoxia. 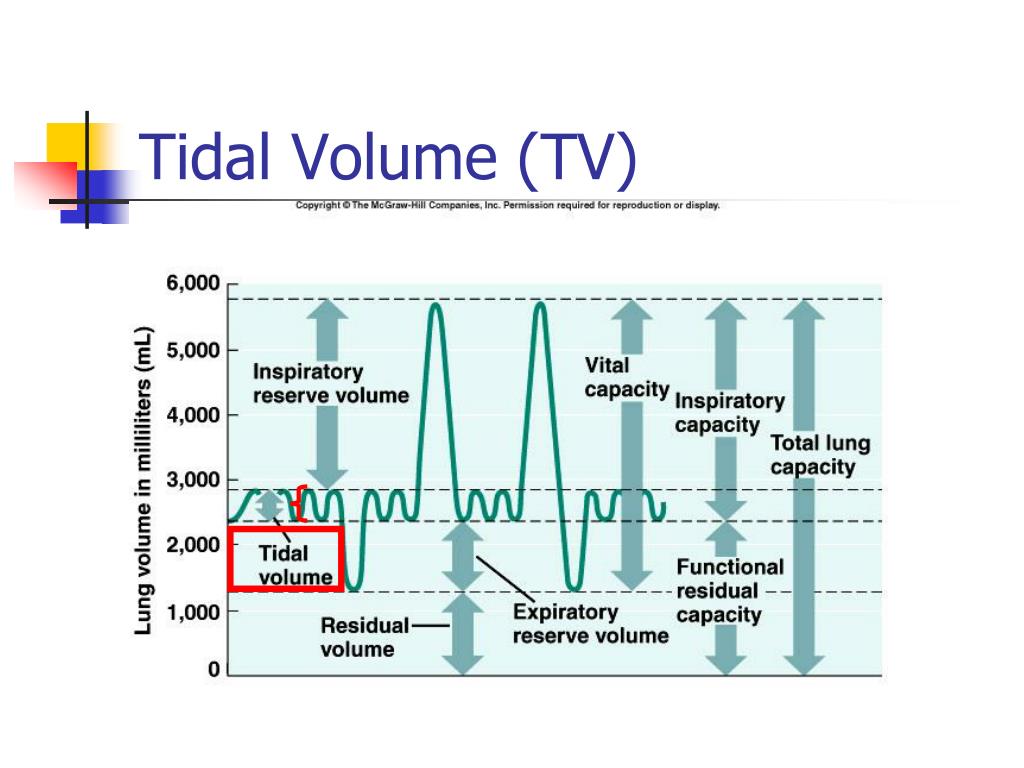
This is important to recognize because providing supplemental oxygen to maintain an SpO2 of 98-100% also can worsen outcomes, even when only maintained for short periods of time. 3 On the other end, if we provide patients with excess supplemental oxygen and maintain high SpO2 levels, they may have significant hyperoxia that goes unrecognized without arterial sampling of the PaO2. We want to ensure we provide adequate supplemental oxygen to prevent hypoxemia and reduce the risk for long-term neuropsychological impairment. It identifies early warning signs of changes in respiratory status and ensures hypoxemic patients receive appropriate supplemental oxygen. Pulse oximetry allows us to continuously and noninvasively monitor the arterial hemoglobin saturation (SpO2) in patients who may have rapidly changing clinical conditions due to respiratory failure. While not immediately apparent as to what is causing the problem, recognizing when something is not quite right is essential and allows for earlier evaluation and treatment. An increase in respiratory effort could be a clue to patient-ventilator dyssynchrony, acidemia, pneumothorax, or other pulmonary or non-pulmonary abnormality. In addition to vital signs and mental status, we must closely monitor the patient’s respiratory effort or work of breathing. Both of these abnormalities are criteria for early detection of sepsis. For example, a therapist detecting a change in mental status with a slight increase in respiratory rate may be a critical early clue to a patient deteriorating. We must take care not to perform each assessment in isolation but rather to evaluate whether the patient’s status has changed over the last several minutes, hours, or even days. Depending on the patient care setting and patient acuity, we may perform this almost continuously or as infrequently as once per shift. With all the advanced monitoring equipment we use, we must not overlook the importance of a focused clinical exam performed by a skilled respiratory therapist. Vital signs, mental status, and respiratory effort Monitoring includes both non-ventilator-specific parameters as well as ventilator monitoring. We will focus on the rationale, accuracy, and effectiveness of preventing harm for each of these monitoring modalities. Respiratory therapists are the front-line care providers for patients requiring mechanical ventilation, especially those in intensive care units or other chronic ventilator units. This goal is crucial during mechanical ventilation, as almost everything we do can cause patient harm. With any patient monitoring system or parameter, our general goal is to identify early warning signs that allow us to reduce or prevent patient harm.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
